Liver Health
Weighing in at around 1.5kg, your liver is your very own chemical factory that works 24 hours a day. It processes virtually everything you eat, drink, breathe or absorb through your skin.
It performs many functions for survival, including detoxification, providing it with energy, the breakdown of red blood cells and substances, helping clot the blood, synthesis of proteins and hormones and storing glycogen. It also holds a reservoir of blood. The liver is a resilient organ that’s easy to ignore. Your liver will continue working even when 75% has been damaged, which often means that it's too late. It can regenerate completely, as long as a minimum of 25 percent of the tissue remains.
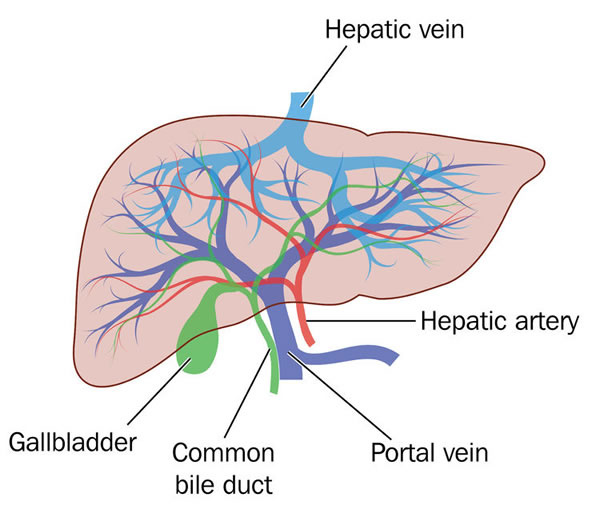
Unlike most organs, the liver has two major sources of blood. The portal vein brings in nutrient-rich blood from the digestive system and the hepatic artery carries oxygenated blood from the heart. The blood vessels divide into small capillaries, with each ending in a lobule (the functional units of the liver). Blood is removed from the liver through three hepatic veins. It is stating the obvious but all the things that the liver needs and all the things that the liver processes have to come via the gut - they have to be absorbed. Your liver needs a rest from both food and toxins, especially alcohol. The absolute best way to do this is from fasting and the second best way is intermittent fasting. Every month take at least 1 or 2 breaks from food. Another great fasting protocol is to do a weekly fast on a 5-2 basis with the five days of eating focused upon clean whole foods. Being properly hydrated with clean water assists liver health and function in many ways. Having sufficient electrolytes is also critical.
The liver performs over 500 functions that are vital to life:
- Cleanses your blood: Metabolising alcohol and other drugs and chemicals. Destroying poisonous substances.
- Regulates your supply of energy: Producing, storing and supplying energy (glucose) to keep your mind alert and your body active. Also produces ketones from fat as a source of energy from fat.
- Produces, stores and exports fat.
- Manufactures many of your essential body proteins involved in: Transporting substances in your blood, clotting of your blood, and providing resistance to infections.
- Regulates the balance of hormones: Including sex hormones, thyroid hormones, cortisone and other adrenal hormones.
- Regulates your cholesterol: Producing cholesterol and converting it to other essential substances.
- Regulates your supply of essential vitamins and minerals. The liver stores vitamins A, D, E, K, and B12. It keeps significant amounts of these vitamins stored. The liver stores iron from hemoglobin in the form of ferritin, ready to make new red blood cells.
- Produces bile: Bile helps the small intestine break down and absorb fats, cholesterol, and some vitamins. Bile consists of bile salts, cholesterol electrolytes, and water.
- Synthesis of the hormone angiotensinogen: This raises blood pressure by narrowing the blood vessels when alerted by production of an enzyme called renin in the kidneys.
Liver diseases
Fascioliasis: This is caused by a parasitic worm known as a liver fluke. They can lie dormant in the liver for months or even years and is a common tropical disease.
Cirrhosis: Scar tissue replaces healthy liver cells. This condition can be caused by a number of factors, including toxins, alcohol, and hepatitis. Alcoholic liver disease is the most common cause of cirrhosis in the world.
Hepatitis: Hepatitis is the name given to an infection of the liver. Viruses, toxins, or an autoimmune response to inflammation can cause it. Hepititis can be reversed and the liver can heal itself. But liver failure can occur in some cases.
Fatty liver disease: In fatty liver disease, fat builds up in the liver cells. If it is not caused by alcohol abuse, the condition is called non-alcoholic fatty liver disease (NAFLD). It is usually caused by genetics, medicines, or a diet high in processed foods that contain fructose. NAFLD is the most common liver disorder in developed countries. Liver cells become insulin resistance. If you eat lots of processed foods and sugars, and eat all day you are very likely to develop a fatty liver. You can be a skinny person and still have a fatty liver.
Liver cancer: The leading causes are alcohol and hepatitis. Liver cancer is the sixth most common form of cancer and the second most frequent cause of cancer death.
Alcohol & the liver
When you drink alcohol, 10% goes to the brain, 10% gets processed in the intestines and the rest (80%) goes straight to the liver to be metabolised. Many beers contain carbs, such as maltose, which also need to be metabolised by the liver or stored as fat. When your body takes in carbs, the glucose gets metabolised throughout the body and only 20% gets to the liver. Drinking alcohol immediately makes your liver work 4 times harder.
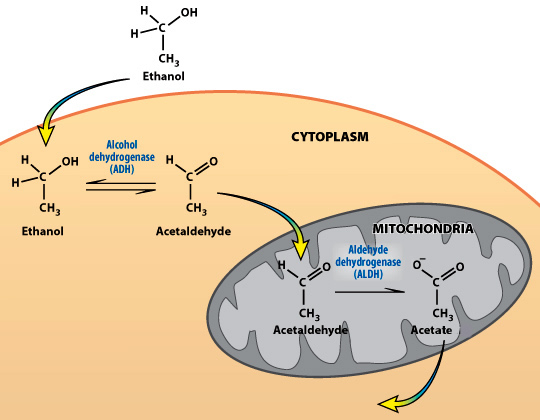
Ethanol does not need insulin to get into the cells, so it diffuses into the liver cells. The liver converts the ethanol to acetaldehyde which is poisonous to the body. It's the acetaldehyde that contributes to a hangover. Acetaldehyde creates "reactive oxygen species" or ROS. These cause tissue and protein damage and make heavy drinkers look older. The mitrochondria in the liver convert acetaldehyde into acetate which is then either:
- Passed into your bodies energy cycle.
- Converted into fat.
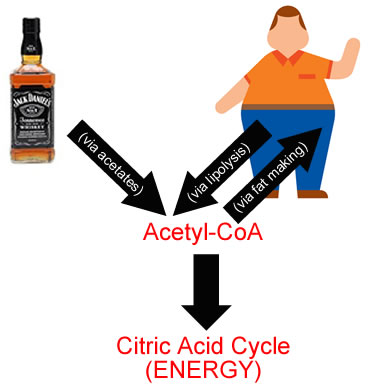
Tons of acetate needs to be processed in the mitochondria by the citric acid cycle. This is then converted into acetyl-CoA which ultimately produces energy, carbon dioxide and water.
Acetyl-CoA can be produced from the alcohol route (via acetate) or via the β-oxidation of fatty acids (fat burning). But when you drink alcohol you are not going to be burning fat! Too much alcohol hitting the liver will put it into overload as you can only convert so much of it to energy (unless you are jogging with a beer!). Your liver has no choice but to take the Acetyl-CoA and start lipogenesis (fat creation).
If you are inactive and drink a lot of booze, or sugary drinks containing high fructose levels, your liver will produce fat as tiny lipid particles. when too many are produced the fat stays inside the liver which then become fatty.
Beer Belly Creation
The fatty acids and cholesterol are gathered by the liver as fatty packages and delivered around the body via the blood. Much of the fat ends up stored in fat tissues, particulary in visceral fat stored around your abdominal organs. Visceral fat is technically excess intra-abdominal adipose tissue accumulation. It's also known as a “deep” fat that is stored further underneath the skin than “subcutaneous” belly fat. It's a form of gel-like fat that's wrapped around major organs, including the liver, pancreas and kidneys.
Many studies have pointed to an association between insulin resistance and visceral fat. Resulting in the increased risk of a number of health problems including type 2 diabetes. Visceral fat secretes a protein called retinol-binding protein 4 (RBP4) which has been shown to increase resistance to insulin.
Fructose + Alcohol is a deadly combination
- Alcohol is processed mainly in the liver.
- Glucose can bypass the liver and be processed throughout the body.
- Fructose can only be processed in the liver.
- Mixers and juices for drinks contain huge amounts of sugar.
Table sugar is 50% glucose and 50% fructose. It is added to all the common mixers. High fructose corn syrup (HFCS55) contains 55% fructose and it is added to juices and drinks. Generally 40%+ alcohols are good because they contain no carbs, but when you mix them with coke, sprite, red bull, tonic water etc, you are going to overload your liver. Your liver will be forced to process 80% of the alcohol and 100% of the fructose from the mixer.
Fructose follows the same pathway as alcohol in the liver. The liver has to work way to hard and it can only dissipate so much energy, so it's going to produce fatty acids and fats via lipogenesis and add to your belly fat. Look at the mixers below, where you can see the grams of sugar in a typical 125ml serving (a small can contains 250ml). A spoonful of sugar weighs 4g so the mixers are adding about 3 spoonfuls of sugar to your drink. Ten whisky & cokes will add 34 spoonfuls of sugar to your body. Not to mention the 1500+ calories!

What things are good for the liver?
- Fasting. Your liver needs a break! It certainly needs a break from alcohol and processed foods. People who start fasting often show an increase in blood lipids because the body has to break down so much fat. But more frequent fasting and intermittent fasting reverses fatty liver disease, reduces liver insulin resistance and reduces inflammation.
- Exercise and movement. You need to move more to get the blood flowing around your body which is going to increase blood flow to and from the liver. Core exercises and stretching and squatting will also move around your abdominal organs, improving blood flow and nerves. Don't be sedentary and especially don't sit for long periods.
- N-Acetyl Cysteine. This is a medication that is used to treat paracetamol overdose. N-acetyl cysteine (NAC) is used by the body to build antioxidants. Antioxidants are vitamins, minerals, and other nutrients that protect and repair cells from damage. NAC is a precursor to glutathione. Taking NAC before you drink is known to reduce the toxic effects of alcohol and reduce your hangover (take least 200 milligrams 30 minutes before you drink). NAC is thought to work even better when combined with thiamine, or vitamin B1. Vitamin B6 may also help to lessen hangover symptoms.
- Vitamin C. Alcohol depletes your vitamin C, which is important for reducing oxidative stress in your liver caused by alcohol. Without high levels of vitamin C in your system, your liver will have to work harder.
- Vitamin D. Vitamin D is typically referred to as a fat soluble vitamin, but actually represents two related fat soluble substances D2 and D3. These molecules are made from 7-dehydrocholesterol, which is activated to vitamin D by UV-B light, in the skin. The liver converts these to to 25-OH vitamin D which then travels to the kidneys to become the active vitamin D3 and vitamin D2. Liver disease leads to impaired absorption of vitamin D.
- Apple cider vinegar. Daily ACV has been scientifically shown to flush the liver, boost circulation and reduce liver inflammation. Apple cider vinegar helps people lose weight and also reduce fat content in the liver.
- Choline protects your liver and can reverse fatty liver disease. Choline plays an important role in the metabolism of fat as an energy source. This action of choline makes it valuable in preventing conditions like fatty liver or excess fat in the blood. Choline’s efficient metabolism of fats has also been linked to a greater level of satiety, which, in turn, leads to a decreased consumption of calories, resulting in overall weight loss. According to an American study, adding choline-rich eggs to breakfast helped obese patients on a low-fat diet lose weight compared to patients who ate a bagel for breakfast with the same number of calories. Choline is abundant in animal liver and egg yolks, but you can cheaply supplement with choline (1-2g is a theraputic dose).
- Eat real, clean foods (preferably organic), including unrefined carbohydrates, vegetables, fruits and healthy fats.
- Anti-inflammatory foods.
- Anti-oxidant foods.
What things are bad for the liver?
- Alcohol, particularly too much in a short period of time.
- Sugary drinks containing fructose.
- Processed foods containing hidden sugars and HFCS.
- Chemicals and toxins:
- Paracetamol/tylenol. Taking too much paracetamol (tylenol) can result in liver damage and even death. Paracetamol is one of the most common causes of poisoning worldwide and the mechanism is the depletion of glutathione and subsequent liver damage. Damage is often irreversible, but doctors actually give patients cysteine (NAC) in an attempt to restore glutathione levels. 50 million Americans take Tylenol each week. This results in 10,000 hospital visits and 500 deaths per year. One in four people frequently exceed the maximum daily dose of 4000mg). Avoid all paracetamol products, they provide minimal benefit and do maximum harm.
- Nonsteroidal anti-inflammatory drugs: Ibuprofen. Naproxen. Diclofenac.
- Birth control pills and synthetic hormones stress the liver and cause benign cysts.
- Anabolic steroids.
- Poly unsaturated fats (PUFAs): PUFAs are very vulnerable to damage from heat, light, and oxygen. Forming lipid peroxides. Eating oxidised fats increases inflammation, and this contributes to most chronic diseases. Your liver will need to work extra hard to combat this extra stress. Vitamin E is the bodies defence against lipid peroxides. Vitamin E is stored in the liver.
- High stress levels are very bad for liver health.
Liver tests
Liver tests are blood tests used to check the health of your liver and your bile ducts. These tests measure the levels of certain enzymes and proteins in your blood, especially enzymes that liver cells release in response to disease.
- Alanine Aminotransferase (ALT) and Aspartate Aminotransferase (AST)
These are liver enzymes normally found in liver cells that leak out of these cells and make their way to the blood when liver cells are injured. The ALT is considered to be a more specific indicator of liver inflammation as AST is also found in other organs such as the heart and muscles. - Alkaline Phosphatase
This is the most frequently used test to detect blockage in the bile ducts. - Bilirubin Test
Bilirubin is a pigment formed primarily from the breakdown of a substance called heme found in red blood cells. It is taken up from the blood, processed, and then secreted into the bile by the liver. There is normally a small amount of bilirubin in the blood in healthy individuals (<17µmol/L). A damaged liver cannot process bilirubin properly which leads to high level of this pigment in the blood. Levels greater than 50 µmol/L are usually noticeable as jaundice. - Albumin Test
Albumin is the main protein which is made by the liver. Chronic liver disease causes a decrease in the amount of albumin produced. - Prothrombin Time and INR
The prothrombin time (also called the “protime” or PT) and the INR are tests used to assess blood clotting. When the liver is injured, clotting proteins are not produced normally.
Sources: liver.ca, draxe.com, drberg.com, ncbi.nlm.nih.gov, loveyourliver.com.au
